As vaccine rollouts take place in many countries around the world, it feels like the globe will soon be able to take a collective sigh of relief that this pandemic could nearly be over. However, the reality may not be so simple. Leading scientists including the chair of the WHO’s strategic and technical advisory group for infectious hazards expect that SARS-CoV-2 will become endemic, circulating amongst the global population on a long-term basis.
The collective devastation of COVID-19 has raised the question of how existing and emerging diseases will continue to affect our global population – and the science is suggesting that outbreaks could become even more frequent and deadlier in the future.
The next big pandemic could be right around the corner.
Dr Mike Ryan, head of the WHO Emergencies Program, recently warned that the next pandemic could be even worse than COVID-19. He predicts that although the fallout from SARS-CoV-2 has been severe, painful and widely devastating, the next disease could be more transmissible and dangerous still. This sentiment has been echoed by Dr Tom Frieden, past Director of the United States’ CDC from 2007 to 2017, as well as communicable disease researchers in Australia and beyond.
Epidemics and pandemics are, statistically speaking, on the rise.
Statistics suggest that we can probably expect another pandemic in the relatively near future, as the occurrence of infectious disease outbreaks is steadily rising along with urban population. EcoHealth Alliance, a New York non-profit research group which tracks disease events globally, reports that the incidence of infectious disease events has more than doubled from the 1940s to 1960s alone. In just the past 20 years there’s been Avian Flu, SARS, Swine Flu, MERS, Avian Flu, Ebola, Zika and COVID-19 to contend with.
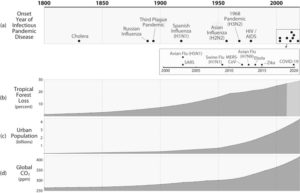
Trends from 1800, collated by Chin, Anne et al in their report
Why are epidemics and pandemics increasing in regularity?
Given that around three out of four new infectious diseases emerge from zoonotic transfer (that is, a virus moving from animals to humans), it makes sense that our impacts on the natural world would be contributing to new infectious diseases. Research has identified several reasons for the rise in outbreaks:
- Increased contact between humans and animals, particularly with wildlife such as bats and primates and with intensively farmed animals such as chickens and pigs. The wildlife trade has been widely identified as a key area that needs to be better managed and controlled.
- Rapid urbanisation, which both raises the human population density and increases the risk of transmission from animals that thrive in these circumstances, such as rats and bats.
- Deforestation, which tends to cause a loss of biodiversity, with the few species that survive tending to host harmful pathogens. A 2020 study showed that deforestation and landscape fragmentation in Uganda led to increased encounters between humans and wild primates.
- Global travel, which increases the speed and ease at which infectious diseases can spread to new areas of the globe. And,
- Climate change, which boosts transmission risk in a variety of ways including increased flooding, the displacement of people to high density camps, and displaced wildlife.
We may already know about some of the biggest threats.
Of course, there are several infectious diseases that are already posing a risk on a wide scale. Tuberculosis causes around 10 million people to fall ill and 1.6 million people to die each year, including in developed countries. Multidrug-resistant tuberculosis is a particular concern and identified by WHO as one of the biggest 10 threats to global health. The question is not if there will be another influenza pandemic, but rather when. An H5N8 strain of avian flu was identified and quickly contained in 2020 on a Russian chicken farm, having jumped for the first time to humans. And then there’s antimicrobial resistance, which is expected to kill 10 million people per year by the time 2050 arrives.
It’s existing threats as well as emerging ones that are posing a risk for our global population. This all appears seriously dire, but there is some good news; globally speaking we’re perhaps more capable than we’ve ever been before to tackle these risks head on.
What’s to be done in preparation?
As Dr Mike Ryan of WHO suggests, let the devastating COVID-19 pandemic be our wake-up call – our warning, so we can start optimising science, logistics, communications, training and governance. The Independent Panel for Pandemic Preparedness and Response published its main report in May 2021, stressing the importance of world governments to remain transparent and proactive about minimising future outbreaks.
Ex-CDC Director Dr Tom Frieden has outlined a number of suggested measures that could help to minimise the impacts of infectious disease on a global scale, including:
- Boosting capacity of countries to quickly identify infectious disease threats, and prepare and respond
- Strengthening international public-health structures including WHO, Global Fund and Gavi
- Working together with wealthier countries and major philanthropies, and
- Encouraging global collaboration to reduce transmission risks and optimise vaccine protection.
Dr Frieden outlines the 7-1-7 strategy for any potential new health threats: to identify the risk within seven days of emergence, to begin investigating and report the event within one day and to launch an effective response within seven days. To do so, we’ll need capable researchers as well as molecular testing equipment that is fast and accurate as well as mobile and accessible. Being able to test on the ground and close to the point of care is key in recognising and responding to threats before they have the chance to wreak havoc on a far larger scale. We’re proud that our Mic magnetic induction cycler and Myra automated liquid handling system are on the frontlines in many parts of the world, helping to do just that.
History shows that epidemics and even pandemics are a part of human existence, but we can also use our most up-to-date scientific awareness and understanding to minimise the impacts of infectious diseases before they put the world on pause and take away more loved ones. Plagues and pandemics throughout the ages are said to have resulted in significant societal, cultural and economic reforms. Let our own changes be productive and proactive, based on facts – and with a focus on the future.
